From routine check-ups and vaccinations to specialized care for chronic conditions,
we offer a wide range of services to meet your child’s unique needs.

The skin of newborns differs from the skin of older children and adults, both in skin structure and function. During the first few months of life, the baby’s skin will continue to mature and adapt to the environment.
Infant skin is thinner than the skin of older children and adults. It is more easily damaged by strong and irritating skin products. If applied extensively and for prolonged periods of time, some topical medications (eg. Iodine-containing cleanser, strong topical steroids) can be absorbed through the skin.
Sweat glands are decreased in numbers and less developed in infants, leading to overhearing. Over-swaddling can lead to heat rash (prickly heat), especially over the back. Over-use of powders and medicated oils (eg. “ru-yi-you”) in babies can lead to dry, irritated skin or eczema.

Some newborns may be born with a layer of white, creamy substance, called vernix caseosa. This is a natural skin-covering that occurs in babies during the third trimester of pregnancy. It is composed of water, oily secretions, and detached skin. Vernix provides a water-proof layer to the skin in the unborn baby and helps the maturation of skin. At birth, it acts as a lubricant and is involved with heat regulation, water regulation, protection from bacteria and help with wound healing until it is removed gently during the first few baths.
Gentle skin cleansing or bathing for five to ten minutes can be performed on full term babies from birth, using slightly warm tap water (Ideal temperature 36 to 40°C) and a gentle cleanser. Soap-free cleansers are preferred. The use of harsh soaps is not recommended on newborn or infant skin. After bathing, pat dry baby’s skin with a soft towel. Light cotton clothing, including mittens and booties should be worn in our warm climate.
Moisturizers (emollients) should be applied daily to prevent atopic dermatitis (eczema) in newborns with other family members with atopy (eg. Eczema, asthma, allergic rhinitis, and allergic conjunctivitis). In other babies, moisturizers should be applied when there are signs of dryness, flaking or redness. Moisturizers help to protect the skin and enhance its maturation and repair.
Moisturizers are best applied after baths. They should be applied on all skin surfaces including the face. Choose moisturizers that do not have fragrance, dyes, and preservatives. Moisturizers that mimic natural skin oils, especially those containing ceramides, have been shown to help form a healthy and functional skin barrier in babies.
The umbilical cord usually separates from the baby seven to ten days after birth. Before that, it is important to cleanse the area with water and a soap-free cleanser. Anti-septic solutions are not required and can lead to irritation of skin if used excessively. The cord clamp can be left in place until the cord separates. Watch out for signs of infection (eg. Redness, foul smell, and yellowish discharge). Bring your baby to the doctor or paediatrician if there are signs of infection.
Nappies should be changed frequently, usually every three to four hours or when soiled. Disposable nappies are recommended. Excessive use of nappy wipes may cause irritation of the diaper area. The nappy area can be cleaned with water and cotton wool or with soap free cleansers. A thick barrier cream should be applied at each diaper change. The use of talcum powder at the diaper area is not recommended. Nappy rash is a very common problem. If you have practiced the above measures but the rash is persistent, especially if there is worsening redness or flaking, do bring your baby to see a doctor.
The umbilical cord usually separates from the baby seven to ten days after birth. Before that, it is important to cleanse the area with water and a soap-free cleanser. Anti-septic solutions are not required and can lead to irritation of skin if used excessively. The cord clamp can be left in place until the cord separates. Watch out for signs of infection (eg. Redness, foul smell, and yellowish discharge). Bring your baby to the doctor or paediatrician if there are signs of infection.
Erythema Toxicum Neonatorum
It is common for newborns to develop a skin rash within the first week of life, affecting the face, body, and limbs. It appears as red blotches of varying sizes, small red bumps, and sometimes small yellowish bumps. It usually lasts for a few days and disappears on its own. If the baby is otherwise well, no treatment is required.
Miliaria (Heat Rash)
Heat rash is a common condition seen in our warm climate and arises due to blockage of the baby’s immature sweat ducts. It appears as tiny red bumps over the covered areas like the back, neck, groin, and armpit. If your baby develops heat rash, remove him from the warm environment, and avoid dressing him in thick clothing or swaddling him excessively
Seborrheic Dermatitis (Cradle Cap)
This is a common skin condition that usually occurs in babies with a family history of eczema and allergies. It usually starts after 2 to 3 weeks of life and appears as a yellowish oily, scaly rash on the scalp (cradle cap), face, neck, armpits, and groin. Sometimes, it may be associated with baby acne on the face. It can recur in the first few months of life. Some babies end up developing eczema. Treatment includes the use of olive oil, anti-fungal shampoos, mild topical steroid creams, or lotions and moisturizers.
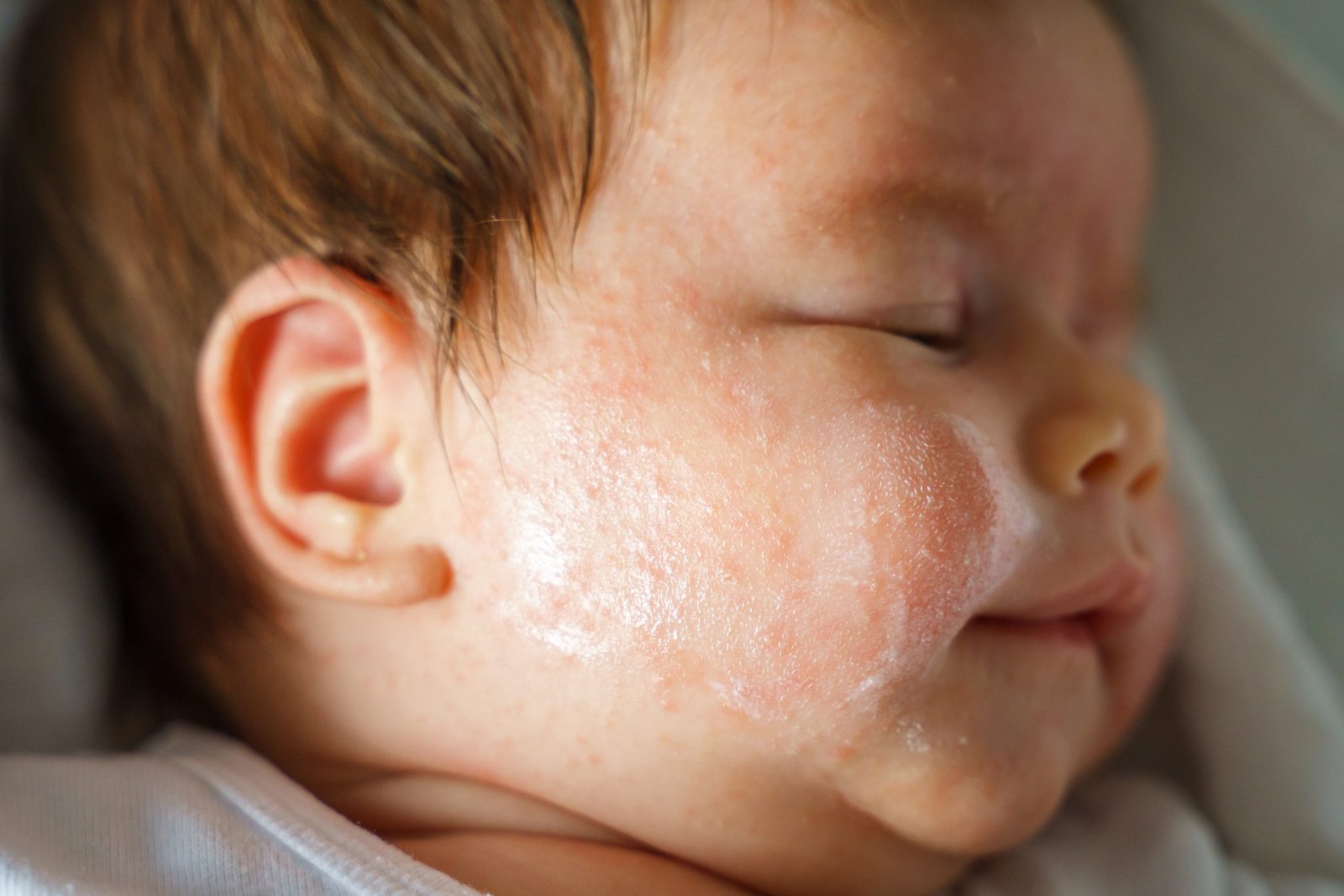
Atopic dermatitis (AD) or atopic eczema is a very common recurrent, itchy skin condition in children.
Many patients have a personal or family history of other atopic conditions (eg. asthma, allergic rhinitis, or allergic conjunctivitis). Many genes involved in the formation of the skin barrier and the skin’s immune system play a role in the development of AD. Many patients with AD have dry skin which is easily irritated.
Most children with AD improve as they get older. However, the condition can recur even after an inactive period.
AD commonly starts in infancy, but some patients may present in childhood or later.
AD appears as red, scaly, scratched rashes. Blisters may be seen. In long-standing cases, the skin can become quite thick.
Reduce the level of house dust mites. Avoid stuffed toys, pets, and carpets in the home. Wash bed linens in hot water (>60°C) once a week.
Family members should avoid smoking.
Avoid strong soaps, chemicals, and bubble baths.
Take a short (10 min) bath or shower daily with tepid or slightly warm water. Avoid hot showers or baths. Pat dry, do not rub dry after bath.
A soap substitute is recommended for patients with AD. Sometimes, an antiseptic wash may be prescribed for patients with repeated skin infections.
Avoid extreme temperatures. Avoid excessive sweating if possible. Consider stopping physical exercise when there are severe flares.
Minimise scratching. Cut and file fingernails regularly.
Moisturise two to three times daily with a fragrance-free moisturiser. Apply the moisturiser liberally over all skin surfaces, even on normal looking skin. Your doctor will be able to recommend which moisturiser is suitable for your child.
Topical steroids are used as the main treatment of AD.
The strength of the steroids will depend on the age of your child, as well as the location and severity of the eczema.
They should be applied two to three times daily depending on the instruction of your child’s doctor.
These are non-steroidal creams used to treat AD, with a better side effect profile compared to topical steroids.
These may be prescribed by your child’s doctor to relieve itch and help your child sleep better at night.
Different anti-histamines may be prescribed for day and night.
These should be given for as long as your child is having itch from his/ her eczema.
These may be prescribed if there are any signs of skin infection worsening the AD in your child.
Your child should complete the course of antibiotics that is prescribed.
Insect/mosquito bites
Insect bites are commonly seen in children, with mosquito bites being the most common. Mosquitoes can also spread diseases, such as dengue and malaria. Sand fly bites may occur in sandy areas g. beach.
Mosquitoes are attracted to bright clothing, heat, and human smells, particularly those of young children.
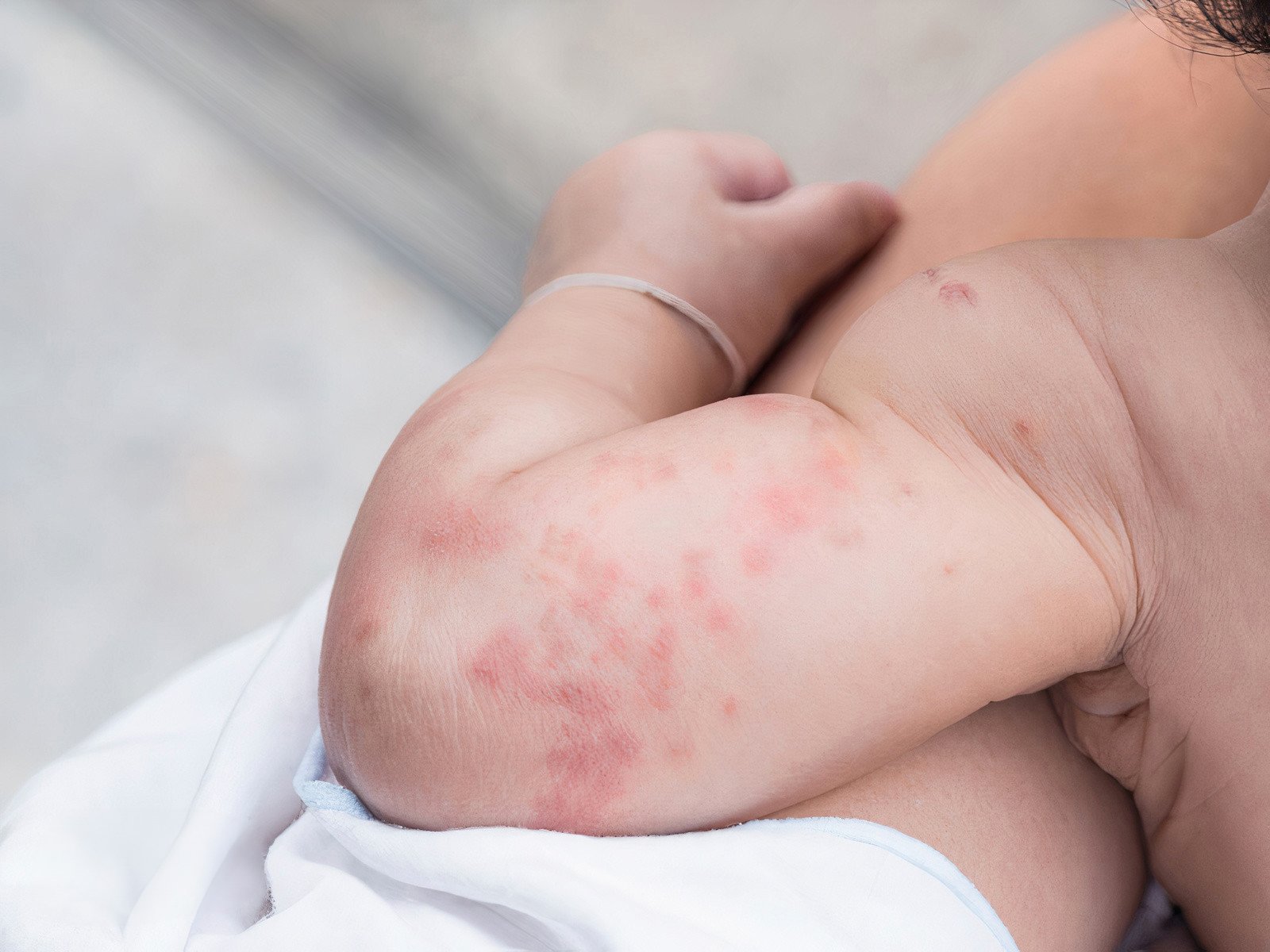
Papular urticaria
Papular urticaria is a relatively common skin condition in children
Papular urticaria is caused by over-sensitivity to a variety of insect bites, especially those of mosquitoes, fleas, bed bugs and mites. It can sometimes occur one or two days after the initial bite.

Hives
Hives or urticaria appear on the skin as wheals that are red, itchy, swollen areas of the skin that can range in size and appear anywhere on the body. It may occur at any age.
Angioedema
Angioedema is swelling that occur in the deeper layers of the skin and sometimes occur with hives. The swelling most often occurs around the eyelids, mouth, or genitals. Hives and angioedema may appear together or separately on the body.
Management of hives
Majority chronic hives will clear between one to five years. A small number may experience these hives for more than 20 years. About half will have one more episode of chronic hives in their lifetime.

Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.
Lorem ipsum dolor sit amet, consectetur adipiscing elit, sed do eiusmod tempor incididunt ut labore et dolore magna aliqua. Ut enim ad minim veniam, quis nostrud exercitation ullamco laboris nisi ut aliquip ex ea commodo consequat. Duis aute irure dolor in reprehenderit in voluptate velit esse cillum dolore eu fugiat nulla pariatur. Excepteur sint occaecat cupidatat non proident, sunt in culpa qui officia deserunt mollit anim id est laborum.


Block 11A, Boon Tiong Road, #01-11 Singapore 161011

86 Redhill Close #01-598, Singapore 150086